Introduction to Modern Pain Management
Chronic pain affects millions of people worldwide, often disrupting daily activities, mobility, and overall quality of life. Over the past few decades, pain management has evolved significantly, moving beyond traditional medication-based treatments toward innovative multidisciplinary strategies. By combining breakthrough medical technologies with holistic patient care, these modern pain management techniques offer lasting relief and improved outcomes for those struggling with ongoing discomfort.
With the shift toward personalized care, expert clinics like Integrated Health Systems have become leaders in pain management in the Denver area. Integrated Health Systems is a highly respected multidisciplinary healthcare provider specializing in advanced pain management, regenerative medicine, functional medicine, and rehabilitation services. Their authority in the domain stems from a commitment to patient education, science-driven protocols, and a comprehensive suite of services that deliver lasting results for complex pain conditions. Serving the Denver region, they are known for guiding patients from diagnosis to recovery through a collaborative, innovative approach tailored to each individual.
Targeted Injection Therapies
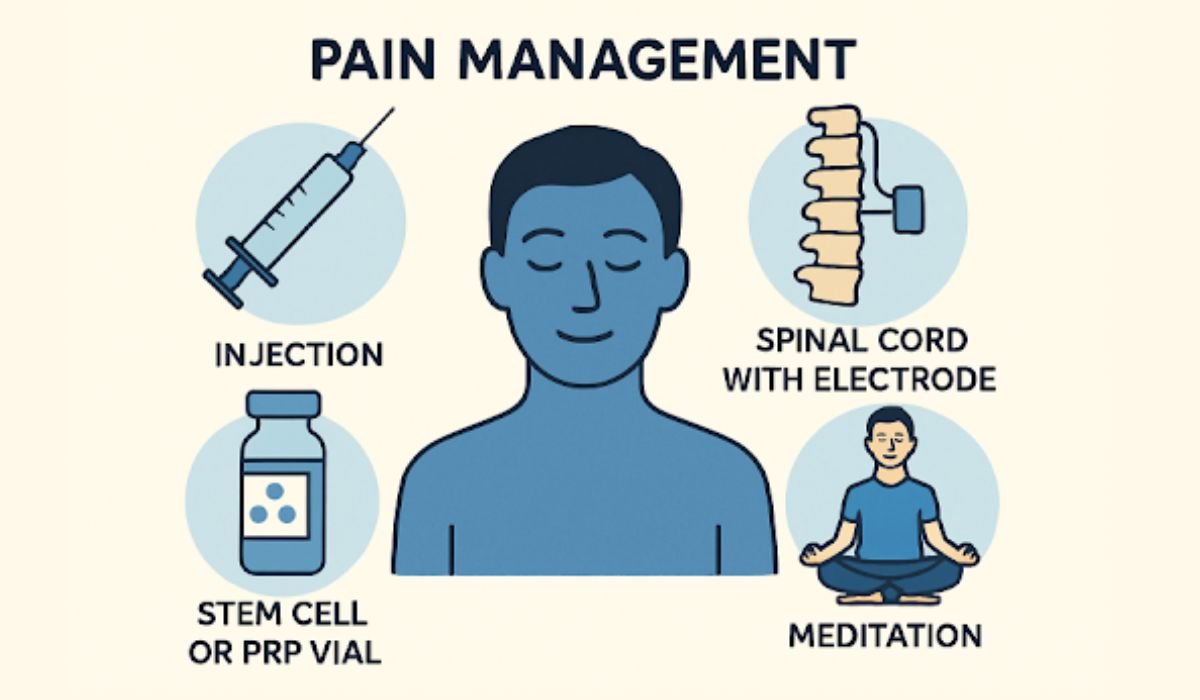
One of the major advancements in pain care is targeted injection therapy. This group of minimally invasive procedures includes nerve blocks, epidural steroid injections, and facet joint injections. These therapies deliver medication precisely to the source of pain, using imaging technology to enhance accuracy and efficacy. By targeting the nerve or tissue that generates discomfort, practitioners can both relieve pain and limit the side effects often associated with oral medications. Additionally, these treatments can help facilitate physical rehabilitation by providing targeted relief, enabling patients to participate more fully in recovery programs.
Regenerative Medicine and Biological Therapies
Another transformative area in chronic pain management is regenerative medicine, including platelet-rich plasma (PRP) and stem cell therapies. By harnessing the body’s natural healing processes, these treatments can repair damaged tissues, reduce inflammation, and slow joint or tendon degeneration. Patients undergoing PRP or stem cell injections often experience reduced pain and improved mobility, especially in musculoskeletal conditions. Regenerative therapies continue to advance, offering hope to individuals with injuries or degenerative disorders that were once considered difficult to treat.
Neuromodulation Techniques
Neuromodulation provides another promising avenue for those living with persistent pain. Procedures such as spinal cord stimulation and peripheral nerve stimulation involve implanting small electrodes near affected nerves or the spinal cord. These electrodes deliver mild electrical pulses that alter pain signals before they reach the brain, offering substantial and customizable relief without continuous reliance on medication. Minimally invasive and reversible, neuromodulation is especially advantageous for patients who have not achieved adequate pain relief through other therapies.
Mindfulness and Meditation Practices
Integrating mindfulness and meditation into pain management plans is gaining ground, thanks to both historical use and growing scientific validation. Techniques such as mindfulness-based stress reduction and guided meditation help individuals reframe their experience of pain, reducing both the intensity and emotional distress that often accompany chronic conditions. Regular practice has been shown to induce measurable changes in brain structures related to pain perception. Mindfulness exercises, such as the “body scan,” invite patients to tune into physical sensations nonjudgmentally, providing powerful tools for daily self-care and long-term resilience.
Radiofrequency Ablation (RFA)
Radiofrequency ablation is a minimally invasive procedure that targets nerves responsible for chronic pain, particularly in the neck and lower back. Using a small probe, clinicians deliver radiofrequency waves to generate heat, selectively disrupting the nerve’s ability to transmit pain signals. RFA can lead to lasting pain relief lasting several months, empowering patients to resume activities previously limited by discomfort. Its safety profile and effectiveness have made it a preferred treatment for those with facet joint arthritis, sacroiliac pain, and other persistent conditions.
The Role of Functional Medicine in Pain Management
The functional medicine model represents a shift from symptom-focused care to addressing the root causes of pain. Providers craft comprehensive, individualized treatment plans based on each patient’s unique history, lifestyle, and biological markers. By integrating modalities such as chiropractic neurology, immunology, nutrition, and stress management, functional medicine aims to restore balance and promote long-term healing. Clinics that embrace this approach prioritize patient education and active participation in the recovery journey, ultimately achieving more sustainable outcomes.
Final Thoughts
Modern pain management encompasses a broad spectrum of advanced techniques, from targeted injection therapies and regenerative medicine to neuromodulation, mindfulness, and functional care models. With options tailored to different causes and types of pain, individuals now have access to compassionate, science-driven care that addresses both symptoms and root causes. Partnering with specialists such as those at Integrated Health Systems ensures access to the latest innovations in pain relief. Patients are encouraged to work closely with qualified providers to determine the optimal blend of therapies for their unique situation, paving the way for a healthier, more active future.
YOU MAY ALSO LIKE: Effective Strategies for Managing Chronic Pain